Introduction to the Prostate:
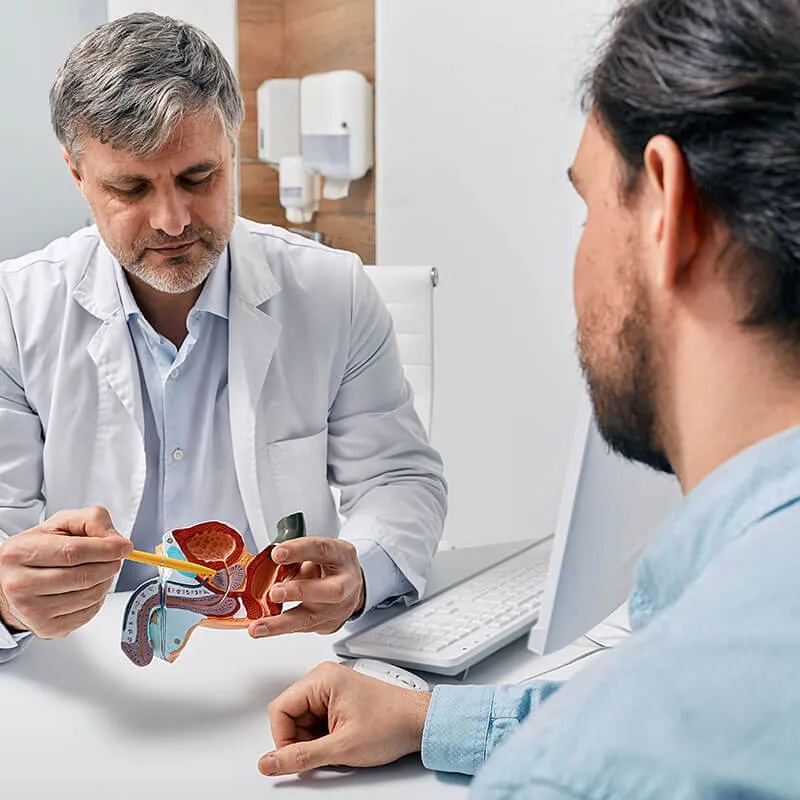
The prostate, a small gland situated below the bladder and in front of the rectum, plays a crucial role in male reproductive health. This web page provides insights into three significant conditions affecting the prostate: Benign Prostatic Hyperplasia (BPH), Prostatitis, and Prostate Cancer. Each condition is explored regarding its causes, symptoms, treatment options, and prevention strategies.Benign Prostatic Hyperplasia (BPH):
Benign Prostatic Hyperplasia (BPH) is a common condition characterized by the non-cancerous enlargement of the prostate gland, which surrounds the urethra. This tube carries urine from the bladder out of the body. While BPH is a benign growth, its enlargement can cause various urinary symptoms, particularly in aging men.Cause:
BPH is a non-cancerous enlargement of the prostate gland, primarily attributed to hormonal changes associated with aging. As men age, the balance of hormones, including testosterone and estrogen, can shift, leading to an overgrowth of prostate tissue.Symptoms:
- Urinary Frequency: Increased need to urinate, especially at night.
- Weak Urinary Stream: Reduced force during urination.
- Urgency: Sudden and intense urge to urinate.
- Incomplete Emptying: Difficulty fully emptying the bladder.
Treatment Options:
- Medications: Alpha-blockers or 5-alpha-reductase inhibitors to relax muscles and shrink the prostate.
- Minimally Invasive Procedures: Transurethral microwave thermotherapy (TUMT) or laser therapy to alleviate symptoms.
- Surgery: Transurethral resection of the prostate (TURP) for significant enlargement.
Prevention:
- Healthy Lifestyle: Regular exercise and a balanced diet can improve prostate health.
- Regular Check-ups: Periodic prostate screenings, especially for men over 50 or those with risk factors.
Prostatitis:
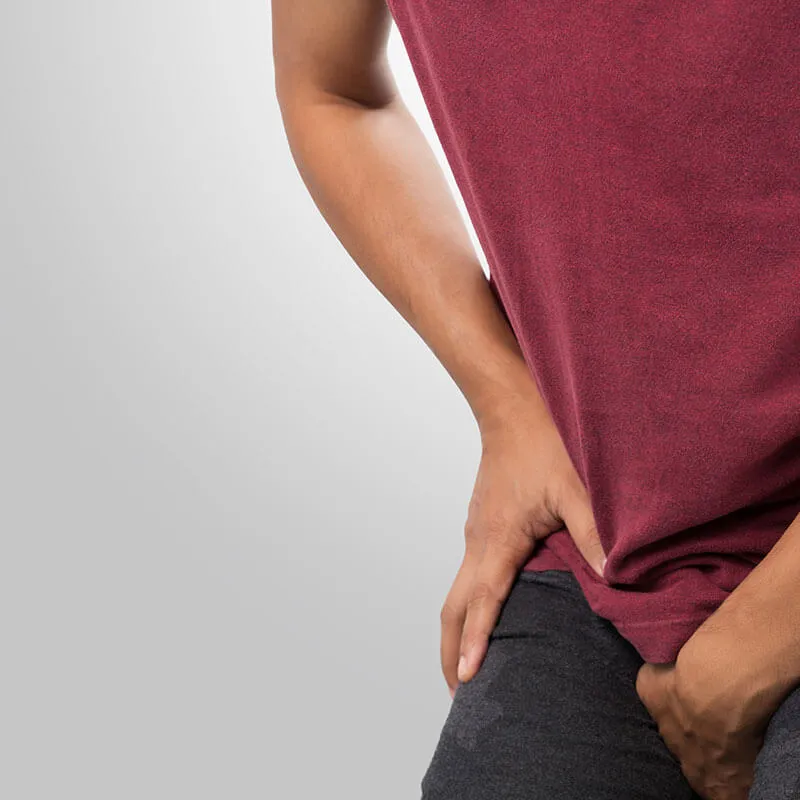
Prostatitis is a medical condition characterized by inflammation of the prostate gland, a small organ situated beneath the bladder and in front of the rectum. This inflammation can lead to various symptoms and discomfort, affecting men of different ages.Cause:
Prostatitis is the inflammation of the prostate gland, often caused by bacterial infection. The exact cause may vary, and non-bacterial prostatitis can also occur, possibly due to immune system responses or pelvic muscle tension.Symptoms:
- Pelvic Pain: Discomfort or pain in the pelvic region.
- Painful Urination: Burning or pain during urination.
- Urinary Urgency: Frequent and urgent need to urinate.
- Fever and Chills: Common in bacterial prostatitis.
Treatment Options:
- Antibiotics: Prescribed for bacterial prostatitis.
- Pain Medications: Alleviate discomfort.
- Alpha-blockers: May help relax prostate muscles.
Prevention:
- Safe Sexual Practices: Practicing safe sex reduces the risk of sexually transmitted infections.
- Regular Prostate Exams: Monitoring prostate health through regular check-ups.
Prostate Cancer:
Prostate cancer is a form of cancer that develops in the prostate, a small walnut-shaped gland in men that produces seminal fluid. It is one of the most common cancers affecting men, typically growing slowly and initially confined to the prostate gland. However, some forms can be aggressive and spread to other body parts.Cause:
Prostate cancer arises when cells in the prostate gland mutate and multiply uncontrollably. The exact cause remains unclear, but factors like age, family history, and genetics may contribute.Symptoms:
- Urinary Changes: Difficulty starting or stopping urine flow.
- Blood in Urine or Semen: The presence of blood is a concerning symptom.
- Pelvic Pain: Discomfort in the pelvic region.

Treatment Options:
- Active Surveillance: Monitoring slow-growing tumors without immediate intervention.
- Surgery: Removal of the prostate gland (prostatectomy).
- Radiation Therapy: Using high-energy beams to target and eliminate cancer cells.
- Hormone Therapy: Lowering testosterone levels to slow cancer growth.
Prevention:
- Healthy Diet: A diet rich in fruits and vegetables and low in saturated fats may lower the risk.
- Regular Exercise: Physical activity contributes to overall health and may reduce prostate cancer risk.
- Screening: Regular prostate-specific antigen (PSA) tests and digital rectal exams (DRE) for early detection.
Conclusion:
Understanding these prostate conditions empowers individuals to make informed decisions about their health. Regular check-ups, a healthy lifestyle, and prompt medical attention for symptoms contribute to maintaining prostate health and overall well-being.What are Prostate Stones?
Prostate stones, also known as prostatic calculi, are small, solid formations that develop within the prostate gland. These stones can vary in size and composition, often containing minerals and cellular debris. Prostate stones are different from kidney or bladder stones and are typically asymptomatic, meaning they don’t always cause noticeable symptoms. Prostate stones may form as a result of calcification of prostatic secretions and can be associated with benign prostatic hyperplasia (BPH) or chronic prostatitis. Schedule Consultation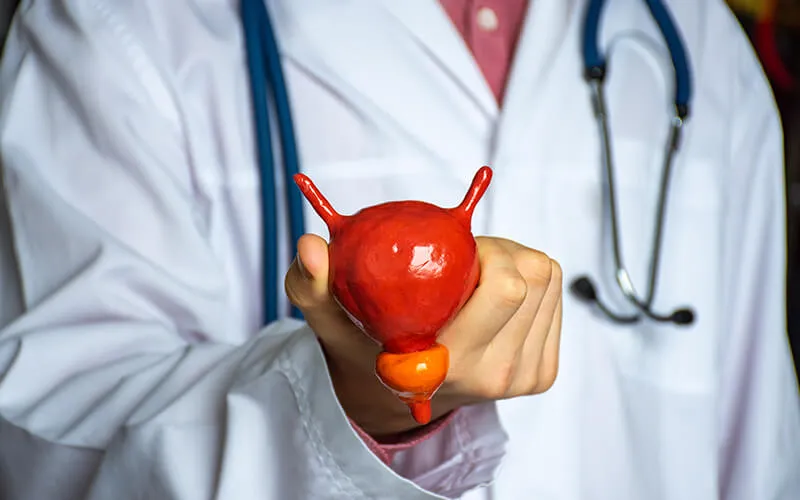
Prostate Stone Symptoms and Signs:
- Prostate stones often do not cause specific symptoms, but in some cases, individuals may experience:
- Pelvic Discomfort: Dull or aching discomfort in the pelvic region.
- Painful Ejaculation: Some individuals may experience pain or discomfort during ejaculation.
- Urinary Symptoms: Prostate stones can be associated with urinary symptoms such as increased frequency or urgency.
Procedures to Manage Prostate Stones:
Management of prostate stones may involve addressing underlying conditions such as BPH or chronic prostatitis. Specific procedures for prostate stones are not commonly performed, as they are often asymptomatic. However, if symptoms are present, treatments may include medications to manage prostate conditions. Schedule Consultation
Causes of Prostate Stones:
The exact cause of prostate stones is not always clear, but they are often associated with:- Benign Prostatic Hyperplasia (BPH)
- Chronic Prostatitis
- Calcification of prostatic secretions