The urinary bladder is a hollow, spherical organ responsible for storing urine.
In general, it has a capacity to hold approximately 500-700 mL, which is
equivalent to about two cups of urine. When the urge to urinate arises, the
muscles in the bladder contract, while the sphincter muscles in the urethra
relax. This coordinated action allows the urine to flow out of the body.
The bladder is a crucial component of the urinary system.
What Are the Basic Functions of Urinary Bladder?
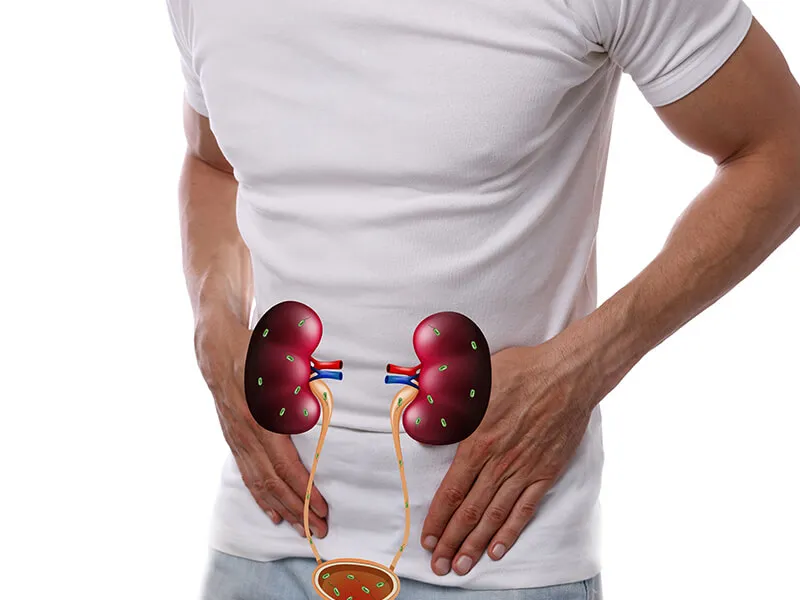
The bladder holds urine, while the kidneys filter blood, removing substances like salt, water, toxins, and waste products, which are then expelled as urine. As the bladder fills, it expands like a balloon. Around 200-350 mL of urine prompts bladder nerves to signal the brain about the need to use the toilet. Emptying the bladder causes it to contract back to its normal size. On average, individuals release about 950-1,900 mL (approximately two quarts) of urine daily. These bodily functions are integral components of the urinary system.Conditions and Disorders
Common conditions that affect the bladder include:
Bladder Cancer/tumor
Bladder cancer is a frequently encountered type of cancer that originates in the cells of the bladder, a hollow muscular organ located in the lower abdomen responsible for storing urine. The majority of bladder cancers start in the urothelial cells lining the interior of the bladder. These cells are also present in the kidneys and the tubes (ureters) linking the kidneys to the bladder. Although urothelial cancer can occur in the kidneys and ureters, it is notably more common in the bladder. Most instances of bladder cancer are detected in their early stages, making them highly treatable. However, even after successful treatment, early-stage bladder cancers may reoccur. Consequently, individuals with bladder cancer typically undergo follow-up tests for several years post-treatment to monitor for any signs of recurrent bladder cancer. These procedures are crucial for maintaining the health and well-being of individuals with a history of bladder cancer.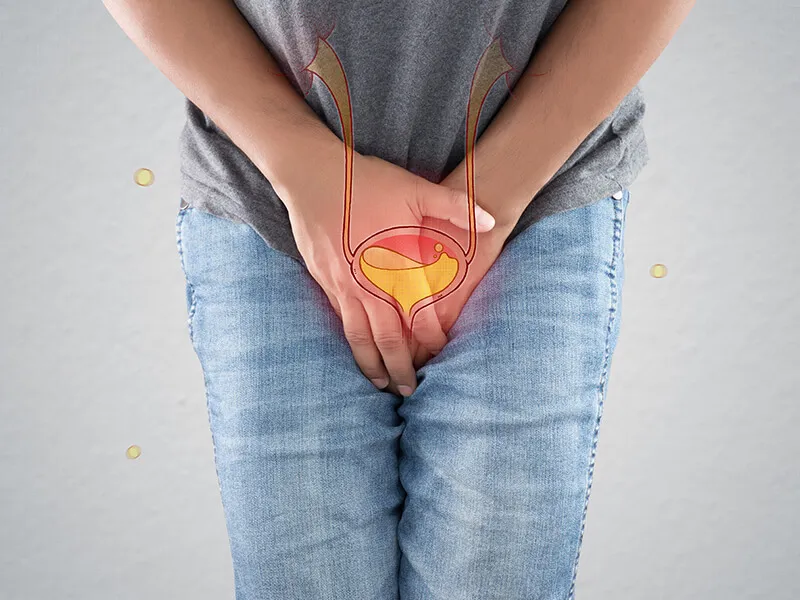
What are Urinary Bladder Stones?
Urinary bladder stones, also known as vesical calculi, are solid formations that develop within the urinary bladder. These stones can vary in size and composition, often containing minerals and salts. Common types include calcium oxalate stones, uric acid stones, and struvite stones. These stones form when there is an imbalance in the substances that make up urine, leading to the crystallization of minerals and salts within the bladder. Schedule ConsultationUrinary Bladder Stone Symptoms and Signs:
Symptoms and signs of urinary bladder stones may include:- Pelvic Pain: Discomfort or pain in the lower abdomen, often concentrated in the pelvic region.
- Hematuria (Blood in Urine): Presence of blood in the urine, giving it a pink, red, or brown color.
- Difficulty and Painful Urination: Struggling or experiencing pain during urination.
- Frequent Urination: Increased urgency to urinate, even with small amounts of urine.
- Cloudy or Foul-Smelling Urine: Changes in the appearance and odor of urine.
- Incomplete Emptying of the Bladder: Feeling as though the bladder is not completely emptied after urination.
Procedures to Treat Urinary Bladder Stones:
Treatment for urinary bladder stones may involve:- Cystolitholapaxy: This procedure involves breaking down and removing bladder stones using a laser or ultrasound.
- Transurethral Cystoscopy: A thin tube with a camera is inserted through the urethra to visualize and remove the stones.
Causes of Urinary Bladder Stones:
Several factors contribute to the development of urinary bladder stones:- Dehydration
- Bladder dysfunction or urinary retention
- Urinary tract infections
- Bladder outlet obstruction
- Foreign bodies in the bladder
- Bladder diverticula
Urinary Bladder Stones Test & Diagnosis:
Medical History and Physical Examination:- Assessment of medical history, symptoms, and physical examination.
- CT Scan (Computed Tomography)
- Ultrasound
- X-rays
- Urinalysis
- Urine Culture
- Blood Tests
- Direct visualization of the bladder using a thin tube with a camera.
- If a bladder stone is removed, its composition can be analyzed for treatment guidance.
When Should You See the Doctor?
If you suspect urinary bladder stones or experience symptoms like pelvic pain, blood in urine, or difficulty urinating, it is important to seek prompt medical attention. Complications such as urinary tract infections or complete obstruction may occur. Regular check-ups are recommended for those with a history of bladder stones or predisposing factors to monitor bladder health. Early diagnosis and appropriate management are crucial for effectively treating urinary bladder stones and preventing their recurrence.
Bladder Cystitis
Cystitis, medically termed as inflammation of the bladder, involves swelling, heat, and potential pain in this part of the body. Typically, cystitis results from a bacterial infection known as a urinary tract infection (UTI), which, besides being painful and bothersome, can pose a serious health risk if it extends to the kidneys. Additionally, cystitis can arise as a response to certain medications, radiation therapy, or irritation from factors like hygiene products, spermicide jelly, or prolonged catheter use. It may also be a complication of other illnesses. For bacterial-induced cystitis, the standard treatment involves the use of antibiotics. However, treatment for other forms depends on the underlying cause. Recognizable signs and symptoms of cystitis include a persistent urge to urinate, pain or a burning sensation during urination, frequent small urination episodes, blood in the urine (hematuria), cloudy or strong-smelling urine, pelvic discomfort, a sense of pressure below the belly button, and occasionally, a low-grade fever. In young children, recurrent daytime wetting incidents may indicate a UTI. It’s important to note that nighttime bed-wetting is generally not linked to a UTI. Seeking prompt medical attention for these symptoms is crucial for effective management and prevention of complications associated with cystitis.
Interstitial cystitis (IC)
Interstitial cystitis (IC) is a chronic condition falling under the category of painful bladder syndrome, causing bladder pressure and pain, ranging from mild discomfort to severe pain. This long-lasting condition primarily affects women, impacting their quality of life. While there’s no cure, various medications and therapies can provide relief. In IC, the signals related to bladder fullness and the urge to urinate become mixed up, leading to more frequent urges with smaller urine volumes than usual. The walls of the bladder become irritated and inflamed, distinguishing it from a normal bladder.Symptoms of interstitial cystitis include
Pelvic pain, persistent urgent need to urinate, frequent urination (up to 60 times a day), and discomfort during bladder filling with relief after urination. Pain during sex and chronic pelvic pain are also common. The severity of symptoms varies, and individuals may experience periods without symptoms. Triggers, such as stress, menstruation, prolonged sitting, exercise, and sexual activity, can cause symptom flares. It’s important to note that while symptoms may resemble those of a chronic urinary tract infection, there’s typically no infection involved. However, symptoms may worsen if a urinary tract infection occurs in conjunction with interstitial cystitis. Seeking medical guidance for proper management is essential.
Bladder Neck Obstruction (BNO),
also known as high bladder neck, is a condition where the passage between the
bladder and urethra narrows or becomes blocked, hindering the normal flow of
urine. This obstruction often leads to various urinary symptoms and can
significantly affect an individual’s daily life.
In BNO, the bladder neck fails to open properly during urination, causing urine
retention and incomplete emptying of the bladder. This can result in symptoms
such as a weak urinary stream, difficulty initiating urination, dribbling after
urination, and a sensation of incomplete bladder emptying.
Men are more commonly affected by bladder neck obstruction, often due to
conditions like benign prostatic hyperplasia (BPH), where the prostate gland
enlarges and compresses the urethra. However, women can also experience BNO due
to factors such as pelvic organ prolapse or prior pelvic surgery.
Symptoms of bladder neck obstruction can vary in severity, ranging from mild
inconvenience to significant urinary retention requiring medical intervention.
Some individuals may experience recurrent urinary tract infections or bladder
stones due to stagnant urine in the bladder.
Certain triggers, such as consuming alcohol or caffeine, taking decongestants or
antihistamines, or being in a seated position for extended periods, can
exacerbate symptoms of bladder neck obstruction.
It’s crucial for individuals experiencing symptoms suggestive of bladder
neck obstruction to seek medical evaluation promptly. Diagnosis typically
involves a physical examination, urine flow tests, and imaging studies such as
ultrasound or cystoscopy to assess the bladder and urinary tract. Treatment
options may include medications to relax the bladder neck muscles, minimally
invasive procedures to widen the bladder neck, or surgery to remove
obstructions.
Managing bladder neck obstruction requires a comprehensive approach tailored to the
individual’s specific needs and medical history. Regular follow-up with
healthcare providers is essential to monitor symptoms, adjust treatment as
necessary, and ensure optimal urinary function and quality of life.

Urinary incontinence
Urinary incontinence Is the loss of bladder control, is a common issue ranging from occasional leaks during activities like coughing to a sudden, strong urge to urinate without reaching a toilet in time. While more prevalent with age, it’s not an inevitable consequence of aging. If it affects daily life, consulting a doctor is crucial. Various types of urinary incontinence include:- Stress incontinence: Leaking urine during activities that apply pressure to the bladder, such as coughing, sneezing, or exercising.
- Urge incontinence: Sudden, intense urges to urinate, often followed by involuntary urine loss. Causes range from minor issues like infections to more serious conditions like neurological disorders or diabetes.
- Overflow incontinence: Frequent dribbling due to an incompletely emptied bladder.
- Functional incontinence: Physical or mental impairments hindering timely toilet access, like severe arthritis affecting quick clothing adjustments.
- Mixed incontinence: Experiencing a combination of stress and urge incontinence